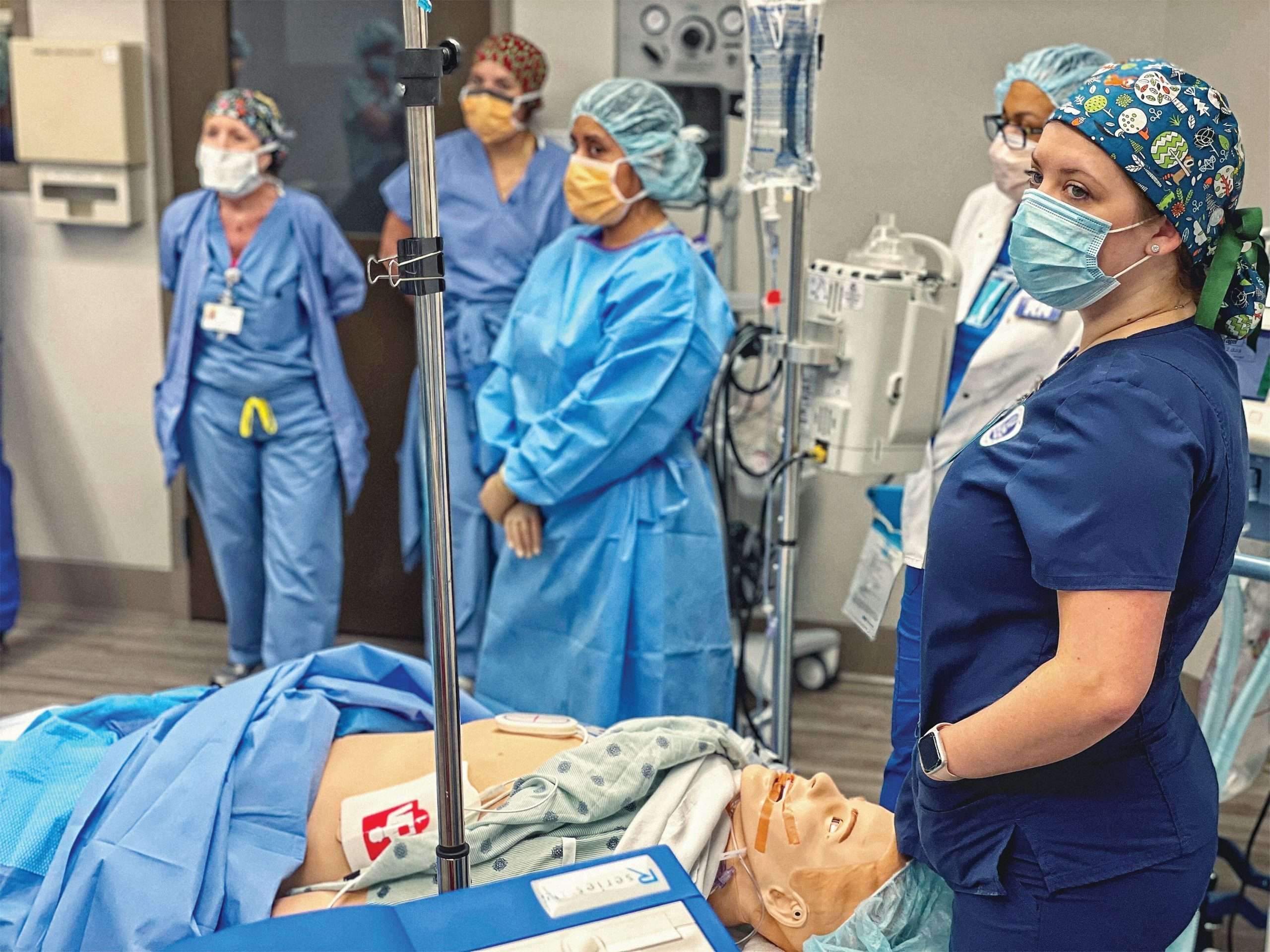
According to a recent report from the Florida Hospital Association, the state of Florida will likely have a shortage of almost 60,000 nurses by 2035. While the nursing shortage has been an ongoing problem for years, the pandemic has accelerated the problem significantly.
“One of the contributing factors is COVID—definitely the burnout factor and the acuity level of the patients. When I look at the critical care numbers, the data is saying that one in three critical care nurses have left their positions. And one out of four nurses have left their positions,” says Kelly Goebel, program director for undergraduate nursing at Florida Gulf Coast University’s Marieb College of Health & Human Services’ School of Nursing. “The secondary piece is that a lot of the staff left for some very lucrative travel nursing positions across the country. So that contributed to our shortage in this area; and that’s what has led to a huge number of nursing shortages and vacancies.”
In addition to the pandemic, Florida’s aging population paired with a continuing influx of new residents is creating even more demand for nurses and health care workers. And unfortunately, filling the demand today, while also planning for increased demand tomorrow, isn’t as simple as just hiring more nurses.
“One of the things that we run into in terms of trying to establish a group of students to serve our community is that we need to increase the numbers in our nursing program,” Goebel says. “The second piece would be finding qualified faculty to teach the students, especially in the Southwest Florida area. We have to have the financial resources to grow a program. I mean, it’s not an instantaneous fix, but you can’t grow a program and produce more nurses and hire more faculty unless you have the resources.”
Given that most nursing schools are still at maximum capacity, another factor fueling the nursing shortage may be a generational one. The issue isn’t that fewer people—especially women—are choosing nursing as a career, but rather that they have more career choices overall.
“I think women over the past 30 years have had more opportunities, and less barriers, to doing other things, besides nursing and being teachers,” says Mary Yankaskas, managing physician, Physicians’ Primary Care of Southwest Florida. “In terms of higher education, going to medical school, going on from nursing school to be a nurse practitioner … there are just so many more options for them.”
Though there are more options for other career paths, Yankaska also believes there are different hindrances today for aspiring nurses. For those who can’t afford to be a full-time student, the biggest issue is simply the cost of living.
“The fact that you almost have to have a smartphone, you have to have the internet. Those kinds of costs of living weren’t there 30 years ago. That becomes a significant barrier for some people,” Yankaskas says. “Being able to have affordable housing, and you’re going to have to commute to school and maybe have a job. It all adds up.”
To help overcome the financial hurdles and ultimately develop more nurses, certified nursing assistants and licensed practical nurses, Yankaskas collaborated with community foundations to develop a new approach. Rather than focusing specifically on nurses, a stair-step plan was encouraged to simply get more health care workers into the system and allow them to find their own niche.
“They started with CNAs (certified nursing assistants), because CNA is more of a stepping stone for most people. It’s a short program … and then they can start working home health or in the hospital. And then they have a job so that they can continue to go on to nursing school to be an LPN or to be an RN,” Yankaskas says. “Health systems (and) the long-term care facilities are always trying to fill those CNA spots. So we got together with the community foundation and partnered with the two local tech schools to increase their enrollment for CNAs and also for medical assistants—also in a shortage for outpatient practices—to help remove barriers to getting their education, be it their applications or uniforms, their drug testing and getting transportation and helping them check off those boxes so they could start school. And that has worked very well.”
Whatever the process, Yankaskas and Goebel agreed that eliminating barriers and expanding opportunities are key to alleviating the nursing shortage. And regardless of the path someone chooses to get into nursing, if they have a passion for it, Goebel believes it will always be a rewarding career choice.
“I say this to my nursing students all the time—and it really is the honest to God truth—but I’ve been a nurse for a really long time and there’s never been one day, not one day, even through a pandemic, when I have ever regretted getting into the nursing profession,” she says. “So, as nurses, we need to keep letting people know how passionate we are and what a great career it is—and hopefully we can get more nurses out there.”
Florida’s nursing shortage by the numbers
21% : Projected growth of Florida’s population by 2035
32% : Population growth of Florida residents between the age of 65 and 74 by 2035
74%: Population growth of Florida residents over the age of 75 by 2035
11,500 and 5,600: RNs and LPNs needed in Florida, respectively, as of 2019
37,400: Projected shortage of RNs in Florida by 2035
21,700: Projected shortage of LPNs in Florida by 2025
2,300 and 1,700: Number of RNs and LPNs, respectively, that would need to enter the workforce each year to meet the projected demand by 2035