Technology has made it easier than ever to order food, drive a car and attend work meetings from the comfort of your couch. The story’s the same for local hospital systems, which are taking advantage of the latest and greatest medical technology to train staff and treat patients. Here’s a look at some of the cool new things going on at local hospitals.
Replicating Real-World Scenarios
Medical professionals need to keep educating themselves on new techniques, technologies and preparation strategies for any scenario that may arise. It’s all in service of treating human patients, but actual human beings often aren’t the best option for learning and practicing skills.
That’s why NCH Healthcare System’s new Judith & Marvin Herb Family Simulation Center is such a game-changer. The only multidisciplinary simulation center between Tampa and Miami, it allows NCH staff to receive vital training and skill refreshing in as close to a real-life setting as possible. Using realistic, high-tech mannequins, staff can run through medical scenarios or procedures in a safe way that comes pretty darn close to an actual encounter with a human patient. “The mannequins can talk, cry, have a seizure,” says Hope Goodwin, the center’s simulation operations manager. “You can use a real-world crash cart and defibrillate them. You can do pretty much anything you can on a real human.”
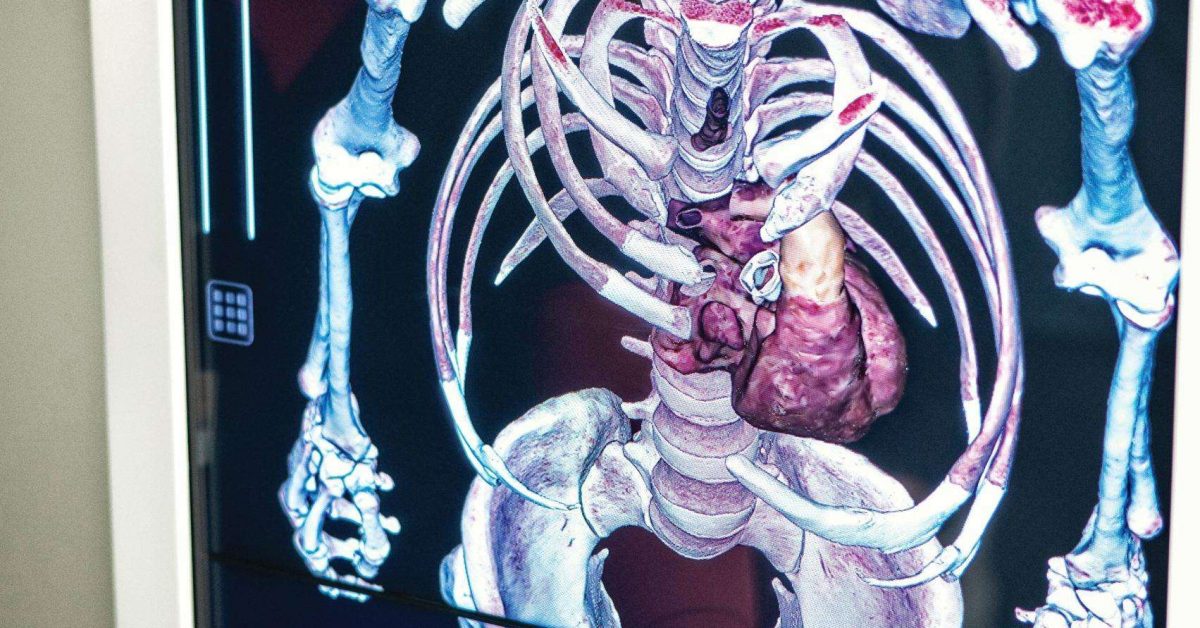
The center’s Anatomage Table serves as another education tool with a major wow factor. “When people walk through the center, it stops them in their tracks,” says Dr. Douglas W. Harrington, the medical director of NCH’s Simulation Center.
The life-size 3D anatomy visualization and virtual dissection tool operates as easily as an iPad and allows users to explore the anatomy the way they would with a cadaver. It’s not only helpful for NCH staff, but can also be used for patient education.
“Instead of a patient being handed a piece of paper about their pacemaker, we can bring the patient over to the Simulation Center and show them on this large-screen TV exactly where the pacemaker is, what it looks like and what would happen if there was an emergency,” says Harrington.
The ultimate goals of all this impressive technology? “Improve efficiencies, improve outcomes and improve patient satisfaction,” says Harrington. NCH’s Simulation Center is currently operating out of an 8,000-square-foot facility and will move into a brand-new, state-of-the-art, 10,000-square-foot space in mid-2022.
New and Notable
Treatment Options
Local hospitals are tapping into new technology to make surgeries and medical treatment easier and more effective for patients. At NCH, surgeons can remove brain tumors by making just a penny-sized incision and using high-tech, microscopic tools, allowing many patients to go home after just 24 hours in the hospital. Spinal surgeries can now be done with incisions the size of a fingernail using an endoscopic approach. 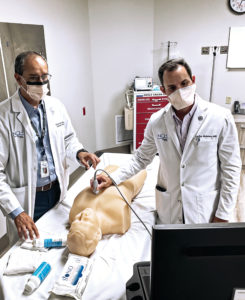
“The principles are the same for both: less blood loss and quicker recovery time,” says Dr. Edison P. Valle Giler, a neurosurgeon at NCH, who said NCH is the only hospital in the area using these techniques and tools. “They’ve been true advancements in neurosurgery.”
Physicians Regional Healthcare System is part of a clinical trial studying Abbott’s Aveir dual-chamber leadless pacemaker. Traditional pacemakers require a surgical incision that can take weeks to fully heal, but this new device is implanted using a much less invasive, catheter-based procedure that has a recovery time of just a few days.
Any patient who needs just a pacemaker (not a defibrillator) is eligible for consideration for the new device, which reduces the risk of infections since it doesn’t require surgical incisions. “It’s very exciting,” says Dr. Kenneth Plunkitt, a clinical cardiac electrophysiologist at Physicians Regional. “We’re one of, I think, maybe a couple of centers in Florida [involved in the trial].”
NCH Healthcare System launched the NCH Research Institute in 2021 to help its physicians take part in cutting-edge clinical trials. The institute “will do so many things for NCH and for Naples, in general,” says Linda Martin, the institute’s director. “The clinical trials will provide the doctors with treatment options not available anywhere except through clinical trials. … We’re seeking to serve physicians in all specialties and support them in advancing their ability to treat their patients.”
The institute is involved in 15 active trials studying such things as the SOLVE-CRT, an implantable device that regulates the heartbeat for patients with heart failure. “It’s about the size of a grain of rice,” says Martin. “This device is amazing.”
There’s an App for That
Patients in need of medical attention can now arrange for an at-home visit thanks to Lee Health’s new partnership with DispatchHealth. Lee County residents can use DispatchHealth’s app or website to schedule in-home visits to address issues ranging from congestive heart failure to eye and viral infections.
The goal of the service is to prevent unnecessary ER visits and hospital admissions. A medical team arrives at a patient’s home within a few hours of the request, with all the tools and equipment needed to assess and treat the issue. If additional medical care is needed, the team coordinates that.
No referrals are required for a patient to use the service, and DispatchHealth accepts a variety of insurances. Lee Health is the only DispatchHealth partner between Tampa and Miami.
“Lee Health is always trying to find innovative ways to provide great care to our community,” says Cindy Drapal, system director of the Neuroscience Service Line for the public health system. “It’s really about getting the patient the care they need quickly so we can help prevent them from being unnecessarily admitted to the hospital.”
Physicians Regional makes use of two apps to more effectively treat stroke patients. The first, a pre-hospital screening tool called Mango developed by Physicians Regional neurointerventional radiologists Dr. Nasser Razack and Dr. Mazen K. AbuAwad, helps paramedics determine whether patients are having a type of stroke caused by a large vessel occlusion (LVO), the cause of most bad outcomes and deaths from stroke.
The second, Viz.ai, uses artificial intelligence to read brain images and determine if a patient has LVO but still has salvageable brain tissue that makes them a candidate for stroke intervention. “It has really increased tremendously the efficiency of stroke diagnosis and treatment,” says Razack. “When you have a stroke, the clock starts ticking. We want to get our patients on the table as soon as possible.”